Telemedicine & Zero-Cast Wx
Posted by Dr Pranesh Kumar
Some clinicians are assessing their patients’ distal radius fracture treatment during COVID-19 using online video communication (FaceTime, ZOOM, etc). Some have found that treating Zero-Cast Wx patients using an online consult is far easier than patients fitted with a conventional arm-cast.
OPEN-CONSTRUCTION | TELEMEDICINE-FRIENDLY | MINIMAL CLINIC TIME
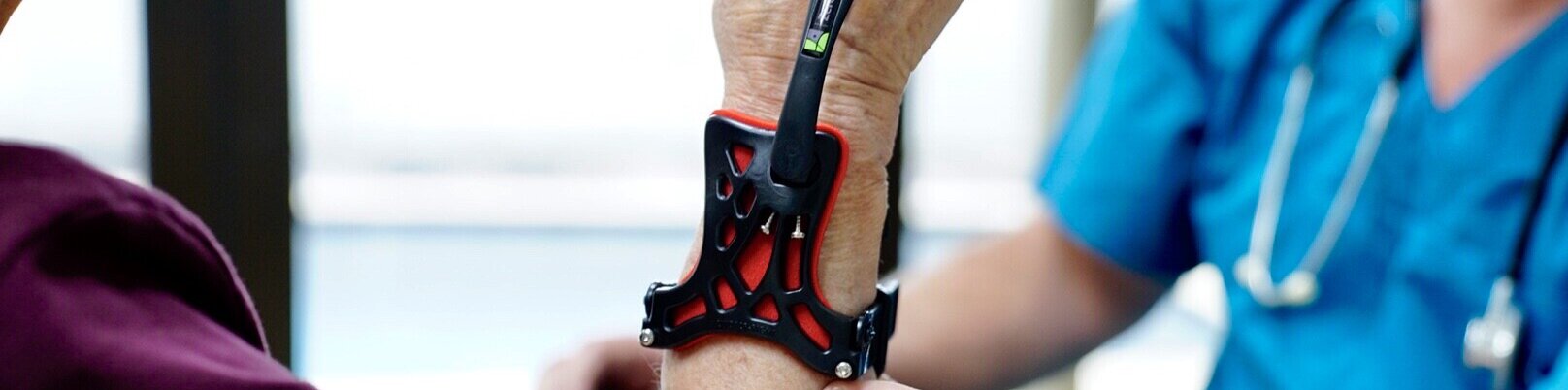
The open-design construction of the Zero-Cast Wx assists with easy visualisation during a tele-medicine consult. The attending clinician can quickly assess any variation from the correct-position of the patient’s Zero-Cast Wx (fitting-check). A typical screen-consult also allows the clinician to perform an accurate assessment of pressure and comfort. Having been assured that effective 3-point fracture stabilization is occurring, the clinician can question the patient and perform a quick check of the skin and device fitting-comfort to ensure that there are no issues with the patient’s ongoing treatment.
As Zero-Cast Wx is radiolucent, patients can be sent straight to x-ray before any clinic-visit. Device-removal is not required prior to the x-ray. This results in a speedy patient flow & reduces time spent at clinic.
EARLY REHABILITATION
Around halfway through the Zero-Cast fracture-treatment (usually around 3 weeks), a clinician can begin to teach their patient a series of basic hand/wrist exercises. This permits the patient to commence early-rehabilitation. Early rehabilitation exercises have been shown to promote tendon-glide and provide improved joint health (wrist joint). During this early rehabilitation, the fracture remains stabilized within the fitted Zero-Cast Wx device. This ensures 3-point fracture fixation of the bone throughout the entire treatment.
When the Zero-Cast Wx is finally removed from patients at the conclusion of treatment, we are hearing anecdotal reports that patients who have undertaken early rehabilitation exercises rarely require further rehabilitation following device removal.
RESULTING COST SAVINGS
Distal radius fractures (DRFs) are one of the most common injuries presenting to emergency clinics throughout the world and a greater understanding of the costs incurred by healthcare providers who routinely treat these injuries has recently been recognised.
A US based study* identified a series of treatment costs that were measured, and the study also highlighted the major cost-drivers when treating DRFs. The study shows that current conservative-treatments (eg. short arm casts) have two identified areas where costs are most significant;
Rehabilitation costs and the indirect costs associated with patient lost work/productivity. Zero-Cast helps to address these specific DRF cost drivers by permitting the following;
- ZERO-CAST Wx allows earlier motion & rehab to occur (promoting healthy tendons and wrist joint)
- Patients with Zero-Cast spend less time in the clinic (rapid-application, no cast-change needed, no plaster-room needed)
- Permits telemedicine assessment (both check-ups & tele-rehabilitation is possible)
- These same drivers associated with cost-reduction offer synonymous benefits during COVID-19
Disclosure; The author of this post (Dr Pranesh Kumar), is the surgeon-designer of Zero-Cast Wx and the founder of the Zero-Cast company.
* Eric Swart, MD, Jacob Tulipan, MD, and Melvin P. Rosenwasser, MD. How Should the Treatment Costs of Distal Radius Fractures Be Measured? The American Journal of Orthopedics® January/February 2017 E54-E59